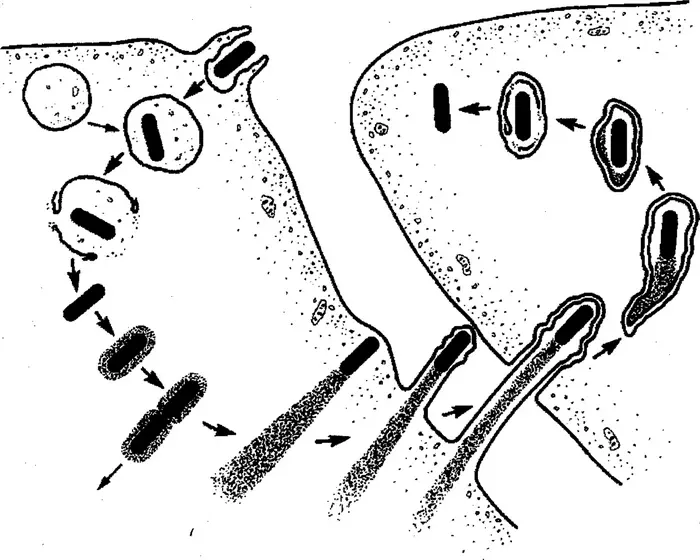
Listeria monocytogenes is, by most reasonable measures, a nasty piece of work. The foodborne pathogen slips into your cells, dodges the immune system’s first line of defence by escaping the very organelle — the phagosome — designed to digest it, then hijacks your own structural proteins to build tiny needle-like protrusions that punch through into neighbouring cells. It is tenacious, cunning and occasionally lethal. It is also, if a team at the University of California, Berkeley has its way, about to become a cancer therapy.
Daniel Portnoy has spent nearly 40 years studying how Listeria gets into our cells and what it does once it’s there. That work has now led to a quadruple-mutant strain, stripped of its ability to cause disease but still potent enough to kick the immune system into a heightened state of alert. The strain is called QUAIL — quadruple attenuated intracellular Listeria — and Portnoy’s startup, Laguna Biotherapeutics, plans to ask the US Food and Drug Administration for clearance to test it in children with leukaemia who have received unmatched bone marrow transplants.
The idea of using Listeria against cancer is not new, exactly. Portnoy first had to figure out how to defang the bacterium, which he did by deleting two genes that it needs to spread from cell to cell. That crippled version, known as LADD, was combined with cancer antigens and trialled in close to 1,000 patients with pancreatic cancer and mesothelioma by a company called Aduro Biotech during the 2000s and 2010s. It didn’t work as well in people as it had in mice. Humans failed to mount the robust cytotoxic T cell response that researchers had been banking on, and Aduro eventually shelved the programme.
But something else showed up in the Aduro data. Alongside the underwhelming T cell results, LADD was triggering a different kind of immune response — one centred on gamma delta T cells, part of the innate immune system rather than the adaptive branch that most immunotherapies target. Gamma delta T cells are generalists. They don’t need to recognise a specific cancer antigen; they go after any cell broadcasting distress signals, whether it has been compromised by a tumour, a virus or a bacterium. Since those early Aduro trials, research by other groups has confirmed that gamma delta T cells can kill cancer cells directly and also rally other immune players like macrophages and natural killer cells.
“The issue is that tumors are a suppressive environment, and so the immune system isn’t really even working,” says Portnoy. “The idea is somewhat similar with Listeria… Listeria itself is seen as foreign and induces an innate immune response, which allows the body to overcome the suppression.”
The trouble with LADD, though, was safety. Even with those two deleted genes, the bacterium could still grow outside cells — in blood, on catheter ports, in the gallbladder. Some patients in the Aduro trials developed systemic listeriosis. That is a serious problem, particularly when you’re treating cancer patients whose immune systems are already battered.
QUAIL solves this by deleting two further genes, ribC and ribF, which encode enzymes the bacterium needs to produce essential cofactors derived from vitamin B2. Those cofactors, FMN and FAD, are plentiful inside mammalian cells, so QUAIL can still grow and provoke an immune response once it enters a cell. But outside cells — in blood, in the gut, on the surface of an implanted port — the cofactors are scarce, and QUAIL simply can’t survive. “We have a strain that can’t grow in blood, it can’t grow in the intestine, it doesn’t grow in the gallbladder… but it grows inside of cells,” Portnoy says. “So that’s the new safer strain, QUAIL.”
In a study published late last year in the journal mBio, Portnoy and colleagues showed that QUAIL was indeed far safer in mice while retaining the immune-stimulating punch of LADD. When placed in sheep blood or human serum, QUAIL numbers dropped continuously, while LADD thrived. On surgically implanted catheters in mice, QUAIL was undetectable at lower doses where LADD colonised readily. In immunocompromised mice lacking B and T cells, QUAIL cleared from the liver entirely within a week; LADD persisted for the full 14 days of the experiment. And crucially, mice vaccinated with QUAIL mounted a protective immune response just as strong as those given LADD.
There is a further twist. Listeria naturally avoids detection by a type of immune cell called MAIT cells — mucosal-associated invariant T cells — because it doesn’t make its own riboflavin. But by engineering QUAIL to express a riboflavin-producing gene borrowed from another bacterium, the team was able to trigger a large expansion of MAIT cells in mice and in human blood cells from 10 healthy donors. MAIT cells have been linked to anti-tumour activity in some cancers, which could give future versions of the therapy an even broader immune kick.
Jonathan Kotula, chief executive of Laguna Bio, reckons the approach stands apart from most cancer immunotherapies precisely because it targets the innate side of the immune system rather than training the adaptive side to recognise a particular tumour. “We believe that if you want to generate a comprehensive immune response, you need to carefully orchestrate the entire immune system,” he says. “And attenuated Listeria seems to be doing that.”
The planned trial at Stanford University Medical Center would use QUAIL in paediatric leukaemia patients after bone marrow transplants, where the hope is that boosted gamma delta T cells could fight off infections, prevent graft-versus-host disease and stop the cancer coming back — all in patients whose adaptive immune systems have been deliberately suppressed. If that goes well, Kotula envisions trials in multiple myeloma, lymphomas, neuroblastoma, sarcomas and solid tumours. Possibly even prophylactic use against intracellular pathogens like malaria and tuberculosis.
All of that is a long way off, mind. QUAIL has been tested in mice, not people. The leap from rodent immunology to human clinical outcomes tripped up LADD once before, and there’s no guarantee it won’t happen again. But there is something appealing about the underlying logic — turn the body’s own alarm system back on, rather than trying to teach it what to look for — and roughly four decades of basic science behind it. Sometimes the best way to fight cancer is with a bacterium that spent millions of years learning how to fight us.
If our reporting has informed or inspired you, please consider making a donation. Every contribution, no matter the size, empowers us to continue delivering accurate, engaging, and trustworthy science and medical news. Thank you for standing with us!